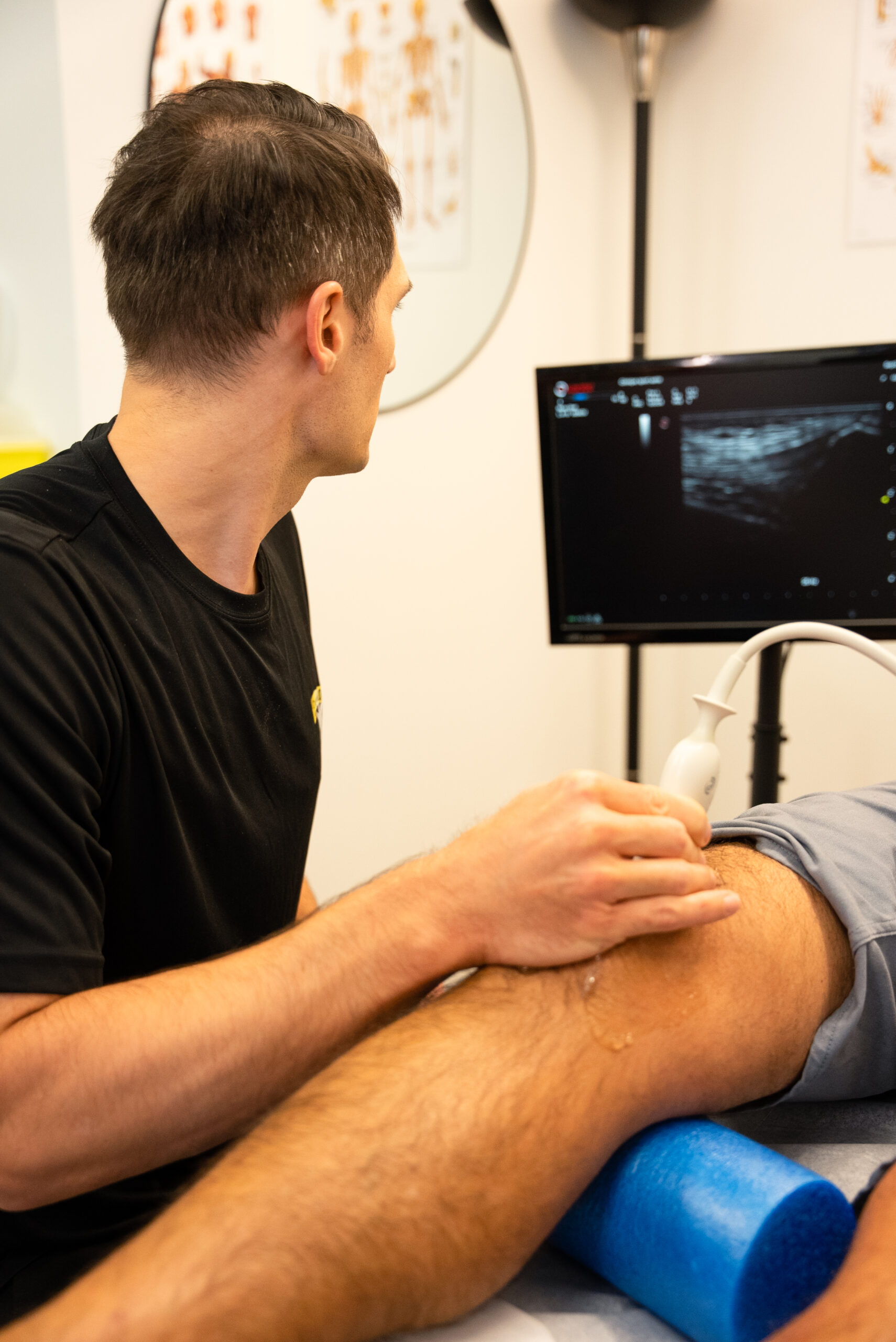
Cortisone injections are one of the most widely used procedures in sports medicine and musculoskeletal care for relieving joint pain and inflammation. Performed in a clinic setting — ideally under ultrasound guidance — they provide targeted relief for many joint and periarticular conditions. This educational guide explains how they work, the indications, the procedure, and the limitations.
What Is a Cortisone Injection?
A cortisone injection (also called a corticosteroid injection) involves injecting an anti-inflammatory medication directly into a joint, bursa, tendon, or tendon sheath. Corticosteroids — such as betamethasone, triamcinolone, or methylprednisolone — are synthetic derivatives of cortisol, a hormone naturally produced by the adrenal glands.
Unlike oral anti-inflammatory medications, cortisone injections act locally, directly at the site of inflammation. This targeted approach delivers high medication concentration to the target site while minimizing systemic effects.
Main Indications
Knee
- Knee osteoarthritis — relief of inflammatory flares with significant effusion and pain
- Prepatellar or infrapatellar bursitis — inflammation of the bursae around the kneecap
- IT band syndrome — lateral knee pain common in runners
- Patellar tendinopathy — tendinopathies of the knee, in selected cases
Shoulder
- Rotator cuff syndrome — tendinopathy or subacromial bursitis
- Subacromial bursitis — one of the most common indications
- Adhesive capsulitis (frozen shoulder) — to reduce inflammation and facilitate physiotherapy
- Calcific tendinitis — sometimes combined with ultrasound-guided calcium lavage
Elbow
- Lateral epicondylitis (tennis elbow) — tennis elbow, for cases resistant to conservative treatment
- Olecranon bursitis — inflammation of the bursa at the elbow tip
Ankle and Foot
- Plantar fasciitis — heel pain, especially with the first steps in the morning
- Retroachilleal bursitis — inflammation behind the Achilles tendon
- Ankle osteoarthritis — relief of inflammatory flares
Cortisone injections are also used for other peripheral joints including the hip (trochanteric bursitis), wrist (De Quervain tenosynovitis), and small joints of the fingers. Learn more about available treatments on our services page.
Procedure Under Ultrasound Guidance
At Clinique Sport Santé Laurentides, all injections are performed under real-time ultrasound guidance. Here is the typical procedure:
- Medical assessment — The doctor reviews your symptoms, physical exam, and available imaging to confirm the clinical indication.
- Positioning — You are comfortably positioned with the treatment area well exposed.
- Aseptic technique — The skin is cleaned with antiseptic solution and a sterile field is established.
- Local anesthesia — In most cases, a local anesthetic is injected first to minimize discomfort.
- Ultrasound guidance — The doctor uses the ultrasound probe to visualize the target structure in real time and guide the needle with precision.
- Corticosteroid injection — The medication is injected directly at the inflammation site.
- Post-procedure observation — You remain briefly for observation and receive clear follow-up instructions.
The entire procedure typically takes 15 to 30 minutes, including the consultation, the procedure itself, and the observation period.
Studies show that ultrasound-guided injections are significantly more accurate than blind injections — accuracy rates jump from 60-70% without guidance to over 95% with ultrasound. Better precision translates to better clinical outcomes.
Duration of Relief: What to Expect
- Short term (1-4 weeks) — Most patients notice significant improvement within 1-2 weeks. A brief pain flare in the 24-48 hours following injection is a normal temporary reaction to the medication.
- Medium term (1-6 months) — For conditions like bursitis or mild-to-moderate osteoarthritis, relief can last 1-6 months.
- Long term — For lasting functional improvement, the injection is ideally combined with a physiotherapy and rehabilitation program.
Generally, no more than 3-4 injections per year in the same joint are recommended to minimize potential tissue effects from repeated use.
When Cortisone Is NOT Recommended
Cortisone injection is not appropriate in all situations. Contraindications include:
- Active local or systemic infection — Risk of spreading infection contraindicates the procedure
- Complete tendon tear — Cortisone in a fully ruptured tendon may further weaken the tissue
- Uncontrolled bleeding disorders or high-dose anticoagulants
- Known allergy to corticosteroids
- Uncontrolled diabetes — Cortisone can temporarily raise blood sugar levels
- Pregnancy — Site-specific individual risk-benefit assessment required
Recovery and Activity Restrictions
- Relative rest 24-48 hours — Avoid intense activities for 1-2 days post-injection. Light daily activities are generally permitted.
- Avoid contact sports and intense effort for 3-5 days
- Ice over the treated area — 15-20 minutes, 2-3 times daily if uncomfortable
- Progressive return to activity — Ideally with physiotherapy follow-up to optimize functional rehabilitation
- Warning signs — Increasing redness, warmth, fever, or significantly worsening pain within 48-72h should be reported to your doctor promptly
Cortisone vs. PRP vs. Viscosupplementation: Educational Comparison
| Treatment | Mechanism | Main Indications | Typical Duration |
|---|---|---|---|
| Cortisone | Potent anti-inflammatory | Bursitis, inflammatory arthritis, inflammatory tendinopathy | 1-6 months |
| PRP (Platelet-Rich Plasma) | Biological growth factors to stimulate tissue healing | Chronic tendinopathies, partial tears, osteoarthritis | 6-18 months (variable) |
| Viscosupplementation (hyaluronic acid) | Joint lubrication and anti-inflammatory properties | Primarily knee osteoarthritis | 6-12 months |
The choice between these treatments depends on clinical factors including the nature and severity of the condition, previous treatment history, and the patient's functional goals. Your sports medicine doctor is the best person to guide this decision based on your individual situation and current scientific evidence.
FAQ — Frequently Asked Questions About Cortisone Injections
Is a cortisone injection painful?
The procedure is generally well-tolerated. Local anesthetic is used first to minimize discomfort. Most patients describe mild pressure rather than pain. A brief pain flare in the 24-48 hours following injection is a normal temporary reaction.
How long does relief last after a cortisone injection?
Typical relief lasts 1-6 months depending on the condition treated and individual response. For some well-localized bursitis, relief may be lasting. For progressive osteoarthritis, repeated injections (maximum 3-4 per year) may be needed.
Can I drive after a cortisone injection?
In most cases yes, especially for upper extremity injections. For knee or ankle injections, mild post-procedure discomfort may affect driving in the first few hours. Discuss your specific situation with your doctor before the procedure.
Can cortisone injections damage tendons?
Reasonable, spaced use of cortisone injections is considered safe according to available scientific data. Frequent repeat injections in the same tendon (more than 3-4 per year) may be associated with increased risk of tissue weakening. This is why a qualified physician evaluates each case individually and respects recommended intervals.
Are ultrasound-guided cortisone injections available in the Laurentians?
Yes. Clinique Sport Santé Laurentides offers real-time ultrasound-guided cortisone injections. To book an evaluation, use our online booking system.
Related Articles
- PRP Injection: Complete Guide
- Knee Viscosupplementation: Complete Guide
- Ankle Sprain: Complete Guide
- Shockwave Therapy (ESWT): Complete Guide